Medication and Older Adults
You are a partner in your health care. This is a partnership between you, your doctor, and your pharmacist. You need to be assertive and knowledgeable about the medications you take.
The Food and Drug Administration is also working to make drugs safer for older adults who consume a large share of the nation’s medications. Adults over age 65 buy 30 percent of all prescription drugs and 40 percent of all over-the-counter medicines.
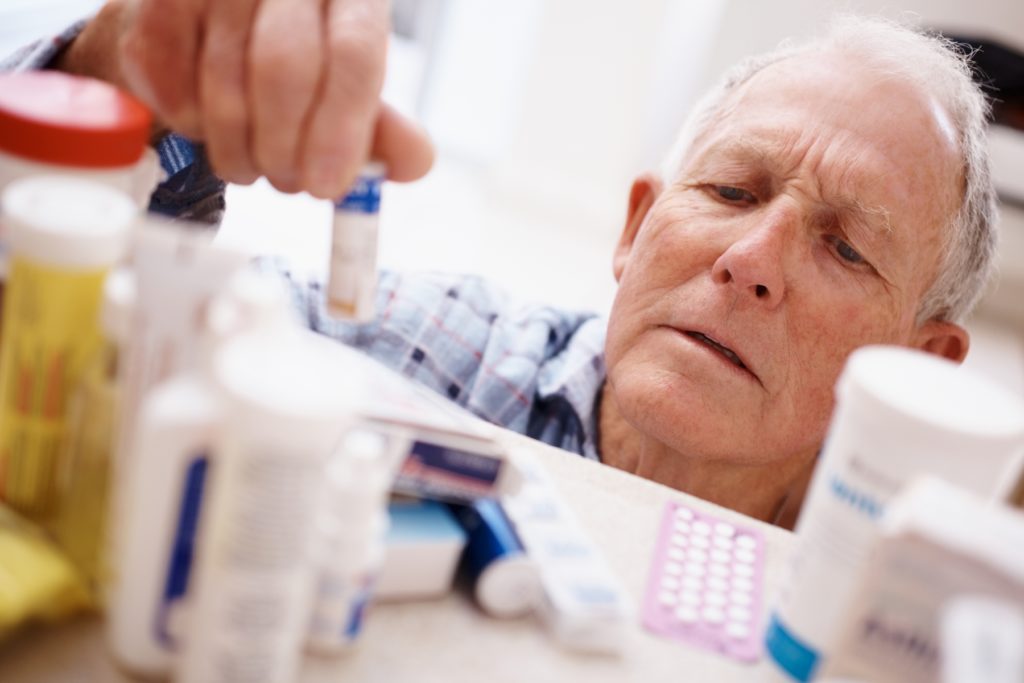
“Almost every drug that comes through FDA [for approval] has been examined for effects in the elderly,” says Robert Temple, M.D., associate director for medical policy in FDA’s Office of Drug Evaluation and Research. “If the manufacturer hasn’t done a study in the elderly, we ask for it.”
More than 15 years ago, the agency established guidelines for drug manufacturers to include more elderly patients in their studies of new drugs. Upper age limits for drugs were eliminated, and even patients who had other health problems were given the green light to participate if they were able. Also, medications known to pass primarily through the liver and kidneys must be studied in patients with malfunctions of those organs. This has a direct benefit for older adults, who are more likely to have these conditions.
In several surveys, FDA discovered that drug manufacturers had been using older adults in their drug studies; however, they weren’t examining that age group for different reactions to the drugs. Now, they do. Today, every new prescription drug has a section in the labeling about its use in the elderly.
Says Temple, “The FDA has done quite a bit and worked fully with academia and industry to change drug testing so that it does analyze the data from elderly patients. We’re quite serious about wanting these analyses.”
When More Isn’t Necessarily Better
Of all the problems older adults face in taking medication, drug interactions are probably the most dangerous. When two or more drugs are mixed in the body, they may interact with each other and produce uncomfortable or even dangerous side effects. This is especially a problem for older adults because they are much more likely to take more than one drug. Two-thirds of adults over age 65 use one or more medications each day, and a quarter of them take three drugs each day.
Not all drug combinations are bad. High blood pressure is often treated with several different drugs in low doses. Unless supervised by a doctor, however, taking a mixture of drugs can be dangerous.

For example, a person who takes a blood-thinning medication for high blood pressure should not combine that with aspirin, which will thin the blood even more. And antacids can interfere with certain drugs for Parkinson’s disease, high blood pressure, and heart disease. Before prescribing any new medication to an older patient, a doctor should be aware of all the other drugs the patient may be taking.
“Too often, older people get more drugs without a reassessment of their previous medications,” says Feinberg. “That can be disastrous.”
There is also evidence that older adults tend to be more sensitive to drugs than younger adults are, due to their generally slower metabolisms and organ functions. As people age, they lose muscle tissue and gain fat tissue, and their digestive systems, liver, and kidney functions slow down. All this affects how a drug will be absorbed into the bloodstream, react in the organs, and how quickly it will be eliminated. The old adage “Start low and go slow” applies especially to the elderly.
Older adults who experience dizziness, constipation, upset stomach, sleep changes, diarrhea, incontinence, blurred vision, mood changes, or a rash after taking a drug should call their doctors.
The following suggestions may also help:
- Don’t take a drug unless absolutely necessary. Try a change in diet or exercise instead. Ask your doctor if there’s anything else you can do besides drug therapy for the condition.
- Tell your doctor about all the drugs you take. If you have several doctors, make sure they all know what the others are prescribing, and ask one doctor (such as an internist or general practitioner) to coordinate your drugs.
- Ask for drugs that treat more than one condition. Blood pressure medicine might also be useful for heart disease, for example.
- Keep track of side effects. New symptoms may not be from old age but from the drug you’re taking. Try another medication if possible until you find one that works for you.
- Learn about your drugs. Find out as much as you can by asking questions and reading the package inserts. Both your doctor and pharmacist should alert you to possible interactions between drugs, how to take any medication properly, and whether there’s a less expensive generic drug available.
- Have your doctor review your drugs. If you take several medications, take them all with you on a doctor’s visit.
- Ask the doctor, “When can I stop taking this drug?” and, “How do we know this drug is still working?”
- Watch your diet. Some drugs are better absorbed with certain foods, and some drugs shouldn’t be taken with certain foods. Ask a pharmacist what foods to take with each drug.
- Follow directions. Read the label every time you take the medication to prevent mistakes and be sure you understand the timing and dosage prescribed.
- Don’t forget. Use a memory aid to help you–a calendar, pillbox, or your system. Whatever works for you is best.
Medicine and Special Needs
Arthritis, poor eyesight, and memory lapses can make it difficult for some older adults to take their medications correctly. Studies have shown that between 40 and 75 percent of older adults don’t take their medications at the right time or in the right amount. About a quarter of all nursing home admissions are due, at least in part, to the inability to take medication correctly.
Several strategies can make taking medication easier. Patients with arthritis can ask the pharmacist for an oversized, easy-to-open bottle. For easier reading, ask for large-type labels. If those are not available, use a magnifying glass and read the name under bright light.
Invent a system to remember medication. Even younger adults have trouble remembering several medications two or three times a day, with and without food. Devise a plan that fits your daily schedule. Some people use meals or bedtime as cues for remembering drugs. Others use charts, calendars, and special weekly pillboxes.
Mary Sloane, 78, keeps track of five medications a day by sorting her pills each evening into separate dishes. One is for morning pills, the other for the next evening. Then she turns each medicine bottle upside down after taking the pill so she can tell immediately if she has taken it that day.
“You have to have a system,” Sloane says. “Because just as soon as I get started taking my pills, the phone rings, and when I come back to it, I think, ‘Now have I taken that?'”
Drug-taking routines should take into account whether the pill works best on an empty or full stomach and whether the doses are adequately spaced. To simplify drug-taking, always ask for the most manageable dosing schedule possible–just once or twice a day, for example.
Severe memory impairments require assistance from family members or professionals. Adult day-care, supervised living facilities, and home health nurses can provide support with drugs.
Active Lives
Not all older adults are in danger of drug interactions and adverse effects. In fact, as more and more people live active lives well into their 80s or beyond, many take few medications at all. Among healthy older adults, medications may have the same physical effects as they do in younger adults. It is primarily when disease interferes that the problems begin.

To guard against potential problems with drugs, however, older adults must be knowledgeable about what they take and how it makes them feel. And they should not hesitate to talk to their doctors or pharmacists about questions and problems they have with a medication.
Says the University of Maryland’s Feinberg: “We need to have educated patients to tell us how the drugs are working.”
Rebecca D. Williams is a writer in Oak Ridge, Tenn.
Cutting Costs
The cost of medications is a severe concern for older adults, most of whom must pay for drugs out of pocket. Even those who have insurance to supplement Medicare must often pay a percentage of the cost of their medicines.
For a new prescription, don’t buy a whole bottle but ask for just a few pills. You may have side effects on the medication and must switch. If you buy only a few, you won’t be stuck with an expensive bottle of medicine you can’t take.
For ongoing conditions, medications are often less expensive in quantities of 100. Only buy large amounts of drugs if you know your body tolerates them well. But be sure you can use all the medication before it passes its expiration date.
Call around for the lowest price. Pharmacy prices can vary greatly. If you find a drug cheaper elsewhere, ask your regular pharmacist if he or she can match the price.
Other ways to make your prescription dollars go further include:
- Ask for a senior citizens discount.
- Ask for a generic equivalent.
- Get drug samples free. Pharmaceutical companies often give samples of drugs to physicians. Tell your doctor you’d be happy to have them. This is especially convenient for trying out a new prescription.
- Buy store-brand or discount brand over-the-counter products. Ask the pharmacist for recommendations.
- Call your local chapter of the American Association for Retired Persons (AARP) and your local disease-related organizations (for diabetes, arthritis, etc.) They may have drugs available at discount prices.
- Try mail order. Mail-order pharmacies can provide bulk medications at discount prices. Use this service only for long-term drug therapy because it takes a few weeks to be delivered. Compare prices before ordering anything.